Cer products have been suggested to be involved in the main mechanisms underlying MS pathology, including those – recently highlighted – driven by B cells. Activation of B cells together with cytokine stimulation promote tissue penetration and destabilization of membrane lipids in CNS, resulting in damage to myelin sheath. SL (in particular Cer derivatives) are essential for maintenance of lipid membranes integrity, so changes in their metabolism and proportion correspond with dynamic processes of demyelination and repair and their pathophysiological consequences22. Although in the aforementioned studies there is convincing evidence for Cer abnormalities in MS, it relies mainly on preclinical models and their translation into human clinical context, with clear identification of Cer related mechanisms of action and potentially relevant MS biomarkers, still remains a challenge4,5,6,7,23. Based on results of our previous studies15,16,17 and scarce literature data11,13,14,24,25, here we focused on particular Cer derivative – C1P, aiming to investigate its putative role as a target and/or mediator of autoimmune response in MS.
C1P, a major metabolite of Cer, can be formed through a stereospecific reaction of phosphorylation, due to direct action of Cer kinase (CerK), while the reverse reaction (conversion of C1P to Cer) is mediated by C1P phosphatase. An appropriate balance between these two molecules is required to ensure cells and tissues homeostasis through regulation of relevant metabolic or signaling pathways. Thus, coordinated action of CerK and C1P phosphatases may have crucial importance for maintaining this balance. Its disturbances with a shift towards accumulation either Cer or C1P may result in metabolic dysregulation, supposedly involved in the background of autoimmune diseases26, neurodegenerative disorders27, cardiovascular illnesses28 or cancer29.
It has been demonstrated that C1P exerts pro-inflammatory properties; however, the underlying mechanisms have not been yet fully elucidated. One of the major function of C1P is its capability to activate cytosolic phospholipase PLA2 (cPLA2), which mediates release of arachidonic acid30– the substrate used for production of eicosanoids, such as prostaglandin E2 (PGE2). This is aligned with the fact that MS patients exhibit higher PGE2 expression/activity in CSF31, lymphocytes32 as well as demyelinative lesions in brain tissue33. A sharp increase of this pro-inflammatory mediator was observed in active stage of MS34, and experimental studies with the use of cyclooxygenase (COX) inhibitors, which oppose C1P action by preventing PGE2 synthesis, suggested their beneficial effect as potential options in MS therapy35.
Other pro-inflammatory activities affected by C1P include: activation of degranulation in mast cells36, stimulation of phagocytosis in neutrophils37, as well as stimulation of macrophage migration38. C1P also increases transport of P-glycoprotein, which regulates the permeability of the blood brain barrier via COX-2/PGE2 signaling39.
On the other hand, it has been shown that C1P might also act as an anti-inflammatory agent, under specific conditions. Anti-apoptotic effects of C1P, promoting cell survival, are related with its ability to block activity of serine palmitoyltransferase40, acid sphingomyelinase41 and TNF-α42. Furthermore, it promotes macrophage chemoattractant protein-1 (MCP-1) release in different types of cells38. Taken together, C1P seems to act on its own rights, executing regulatory effects and modulating cell functions depending on circumstances.
Although C1P has been reported to exert anti-inflammatory and homeostatic functions in neural tissues, accumulating evidence indicates that SL metabolism is profoundly altered during neuroinflammatory and neurodegenerative processes. Dysregulation of Cer–SL pathways has been widely documented in MS and other neurodegenerative disorders, including alterations in Cer, sphingosine-1-phosphate, and related lipid mediators, which are tightly linked to immune activation and neuroinflammation10,43,44,45,46,47. C1P itself is recognized as a bioactive lipid involved in the regulation of inflammatory signaling pathways, immune cell migration, and phospholipase A2 activation, placing it at the interface between lipid metabolism and immune regulation38,48,49. We therefore propose that increased anti-C1P IgG levels observed in RRMS patients reflect a secondary immune response to neuroinflammation-driven alterations in SL metabolism rather than a primary pathogenic mechanism. Local dysregulation of Cer and C1P turnover in the inflamed CNS may lead to abnormal exposure or release of C1P-containing membrane domains, promoting the formation of lipid neoepitopes and subsequent induction of a humoral immune response. This interpretation is further supported by previous reports demonstrating the presence of autoantibodies against lipid and glycolipid antigens in MS and other neuroinflammatory diseases, including antibodies directed against phospholipids, gangliosides, sulfatides, and myelin-associated lipid complexes50,51,52. In this context, anti-C1P antibodies are more likely to represent biomarkers of active neuroinflammatory processes rather than direct drivers of disease pathology.
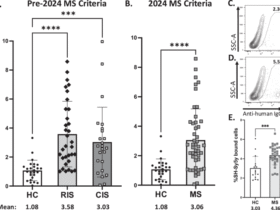
In one of the previous reports by our team members, an increase in C1P subspecies (mainly C18:1-C1P and C24:1-C1P) was demonstrated in inactive MS lesions in comparison with specimens representing other CNS disorders or normal brain tissue. On the contrary, active MS plaques were characterized by a significant decrease of C1P subspecies16. The studied autopsy samples from MS subjects represented advanced stage of disease, associated with chronic inflammation and presumably extensive neurodegenerative component. In the present study we focused on earlier phase of the disease (i.e. RRMS), when active immune-mediated inflammation is a predominating mechanism of CNS injury – therefore antibodies as markers of autoimmune humoral response were chosen as the subject of investigation. The main findings presented here included elevated levels of nearly all analyzed anti-C1P IgG in serum of RRMS patients in comparison to HS, with the highest computed effect size (r = 0.61), denoted in Table 2 as large, for anti-C24:1-C1P (Fig. 2E). There is a striking consistency in the results from both studies, despite differences in MS stages and studied material (brain tissues vs. serum). Translation of metabolomic profiles in autopsy tissue samples into presence of targeted antibodies in body fluids from patients with active disease is extremely complex and requires analysis of many associated factors (i.a. changing dynamics of metabolic processes in the course of disease and compartmentalization of inflammatory process within CNS during its late stages). It can be hypothesized that each stage of MS is associated with the concerted action of Cer derivatives (perhaps with most relevant role of C1P), with their changing interactions in this pathological cross-talk.
It should be mentioned that the level of IgG anti-C24:1-C1P was significantly lower in both RRMS subgroups in relation to NI-OND only (Supplemental Fig. S3, panel E), whereas the level of IgG anti-C24:0-C1P in both RRMS subgroups was significantly lower than in both OND subgroups (Supplemental Fig. S3, panel D). Overall, these results suggest that increased humoral response against long-chain C1P subspecies is particularly specific for MS and it does not just reflect overall neuronal injury or dysregulated immune-mediated inflammation in CNS. However, comparisons between RRMS and OND subgroups have to be interpreted cautiously. I-OND subgroup comprised patients with immune-mediated disorders (vasculitis and chronic polyneuropathy), which share inflammatory background with MS but differ in source of autoreactive humoral response (intrathecal Ig synthesis in MS). NI-OND subgroup was more heterogenous (migraine, cerebrovascular disease and hydrocephalus) which might have affected the results in view of small sample size. In further exploration, involvement of larger groups representing particular neurological conditions, with or without inflammatory component, would enable more precise analysis of these relationships. Importantly, the reliability of the above findings was supported by eliminated impact of immunosuppressive/immunomodulatory drugs, as the patients were included in the study prior to such treatment or after appropriate wash-out period.
There is an evidence that fatty acid chain length of Cer can determine biophysical properties of this SL mediator53. In physiological conditions, medium chain Cer (C16 and C18) are known to be enriched in cerebral gray matter, while long chain ones (C24) – in white matter and myelin sheath54. Considering distribution of Cer derivatives in the brain, presence of the medium chain ones would reflect neuronal injury55, while the long chain ones – oligodendrocytes degradation15. The long chain Cer (C24) are also known to be the major Cer subspecies present in serum/plasma whereas C1P constitute only 0.15% of all SL components56. However, it should be taken into account that the pattern of anti-Cer IgG in body fluids, revealed by our previous study17 reflected metabolic perturbations of Cer, supposed to occur due to processes involved in MS background. The anti-Cer IgG alterations in serum (unlike in the CSF) were observed only for Cer containing medium chains (C16:0-, C18:0- and C18:1-Cer) with no change for the long chain ones17. Current findings revealed altered patterns of IgG against C1P in serum of RRMS patients. Here we found that anti-C16:0-C1P (Fig. 2A), anti-C18:0-C1P (Fig. 2B), anti-C18:1-C1P (Fig. 2C) and anti-C24:1-C1P (Fig. 2E) serum IgG levels were increased in RRMS patients in comparison with HS group. In turn, levels of IgG against C16:0-C1P (Fig. 2A), anti-C18:1-C1P (Fig. 2C), C24:0-C1P (Fig. 2D) and C24:1-C1P (Fig. 2E) were decreased in RRMS in relation to OND (including distinguished subgroup of inflammatory ones). There were not significant differences between RRMS and HS group in the case of anti-C24:0-C1P (padj=0.903) and between RRMS and OND for anti-C18:0-C1P (padj=0.725). What is more, the calculated effect sizes were negligible (r < 0.04) which would suggest some similarities between groups. Nevertheless, due to small sample sizes considered in this study, this phenomenon requires further investigations. In addition, the results of ROC analysis indicated that the determination of anti-C18:0-C1P and anti-C24:1-C1P serum IgG levels might be useful for discriminating RRMS from HS group (Fig. 3, panel C and G), whereas anti-C16:0-C1P and anti-C24:0-C1P serum IgG levels – for discriminating RRMS from OND group (Fig. 3, panel B and F). In these cases, there were relatively high values of PPV− between 0.773 and 1.0 (see Table 3). They suggest that proposed classifiers have a strong tendency to decrease the level of false positive errors meaning that less subjects will be inappropriately diagnosed with RRMS. Furthermore, the usefulness of the above anti-C1P IgG subsets in distinguishing pathological from physiological conditions, as well as disorders with different etiology, was confirmed by means of multivariate statistical method of cluster analysis (Supplemental Fig. S7 and S8). Despite somehow subjective selection of variables for clustering and the number of clusters (justified by the results of initial analysis), the findings from this multivariate technique support the concept that panels/sets of anti-C1P IgG may be of greater discriminating value than single immunological parameters (Fig. 4). Such a panel including anti-C16:0-C1P, anti-C18:0-C1P, anti-C24:0-C1P and anti-C24:1-C1P IgG might be considered for further investigation towards potential clinical implications – the use of anti-C1P IgG as biomarkers in differential diagnosis at MS onset, especially in atypical cases.
In recent years, specific autoantibodies (IgG anti-AQP4 and anti-MOG) have been revealed as pathological hallmarks specific for neuromyelitis optica spectrum disorders (NMOSD) and anti-MOG Abs associated disease (MOGAD), currently used as their core diagnostic biomarkers. However, no such biomarkers have been identified for MS so far. Neurofilaments light chains (Nfl) and glial fibrillary acidic protein (GFAP) are considered as reliable indicators of MS activity and/or progression but their specificity is very low as they reflect neuronal injury and astroglial reactivity in various CNS diseases, independent from their background. Thus additional biomarkers helpful in discriminating MS from other CNS diseases are being extensively sought8.
Few attempts have been made to use anti-Cer antibodies as biomarkers of activity in other disorders, including those of the nervous system. In leprosy, presence of anti-Cer antibodies was found to be related to extent of nerve sheath damage and particular bacterial strains as pathogenic factors57. In the rare autoimmune condition, encephalomyeloradiculoneuropathy (EMRN), accumulation of species-specific Cer (mainly long chain ones) was demonstrated in CSF and presence of anti-neutral glycolipids antibodies – in CSF and serum. Profile of these antibodies allowed to differentiate patients with ERMN from the reference group with Parkinson disease, and their titers decreased after effective immunomodulatory treatment. Dysregulation of glycolipids metabolism and its impact upon invariant natural killer T cell development, as well as abnormal complement activation, were suggested to play a relevant role in EMRN pathophysiology54,58. Furthermore, in non-small-cell lung cancer (NSCLC) anti-Cer antibodies were supposed to be produced by the tumor and its microenvironment, and to neutralize pro-apoptotic effect of Cer. Significantly elevated levels of anti-Cer antibodies were revealed in serum and bronchial wash fluid samples from NSCLC group (in comparison with HS) and they showed a tendency (though not significant) for prolonged overall survival59.
Evaluation of activity in MS has been so far based on clinical assessment and radiological indices (new and/or contrast-enhanced lesions in MRI). However, there is an ongoing search for specific and reliable body fluid biomarkers of disease activity8. In view of our previous findings, Cer derivatives and antibodies against them seemed promising candidates for the role of such biomarkers. Following more precise analysis of RRMS subgroups, no significant differences in anti-C1P IgG levels were found between those in relapse or in remission. No correlations were revealed between these IgG levels and disease duration, EDSS score and Link index, either.
Although no relationships were found in our study group between immunological measures and MS-related clinical data (Supplemental Fig. S9), potential clinical utility of these findings should not be discredited. The group was characterized by a relatively short MS duration and mild disability, and marked individual differences in disease course in MS populations must be taken into account. Perhaps in a larger group of patients and in prospective observation these relationships would appear more relevant.
Indeed, a small sample size constitutes a limitation of our study, with regard to the study design including comparative analysis of multiple subgroups. However, statistical models applied in the analyses were meant to mitigate these constraints. Furthermore, because of focusing on RRMS only, the results of the study may not accurately reflect abnormalities in SL metabolic pathways in different types and stages of the disease. Another limitation is associated with the fact that anti-C1P IgG presence was determined only in serum and not in CSF. Nevertheless, in view of long-term course of MS and need for regular follow-up, serum/plasma biomarkers are much desired due to their better availability. Based on experiences with other body fluid biomarkers, their serum level may adequately reflect their production in CNS8. There is also some evidence that peripheral blood may contribute to formation of immune complexes due to selective transport and the blood-brain barrier (BBB) leakage60.
To our best knowledge, this study for the first time focuses on the presence and meaning of anti-C1P antibodies in serum of MS patients. Strengths of the study include also complex statistical approach (combined ROC and cluster analysis) which allowed comprehensive presentation of relevant findings, as well as evaluation of links between immunological and clinical data. These results shed some light on the perturbation on SL metabolism (especially significance of balance between Cer and C1P) in the background of neurological diseases, specifically MS, encouraging further targeted investigations in this field. Our findings support the concept of altered Cer metabolism as a target and/or mediator of autoimmune response in MS. Nevertheless, potential value of antibodies anti-C1P subclasses as diagnostic biomarkers or measures of MS activity warrants verification in larger groups of MS patients, preferably in prospective observation. Furthermore, profile of selected anti-C1P IgG should be assessed parallel in blood and CSF, with thorough analysis of links between these two compartments and their contributing factors. Hopefully, these studies will lead to a better understanding of the role of this intriguing phosphosphingolipid in pathophysiology of MS, with emerging clinical implications.















Leave a Reply