Key Takeaways
- Autoimmune hives are itchy, red bumps on the skin that can last for months or years due to the immune system attacking healthy cells.
- Some people may have symptoms of a co-occurring condition, like thyroid disease.
- Stress can cause or worsen hives, so practices like mindfulness and exercise might help.
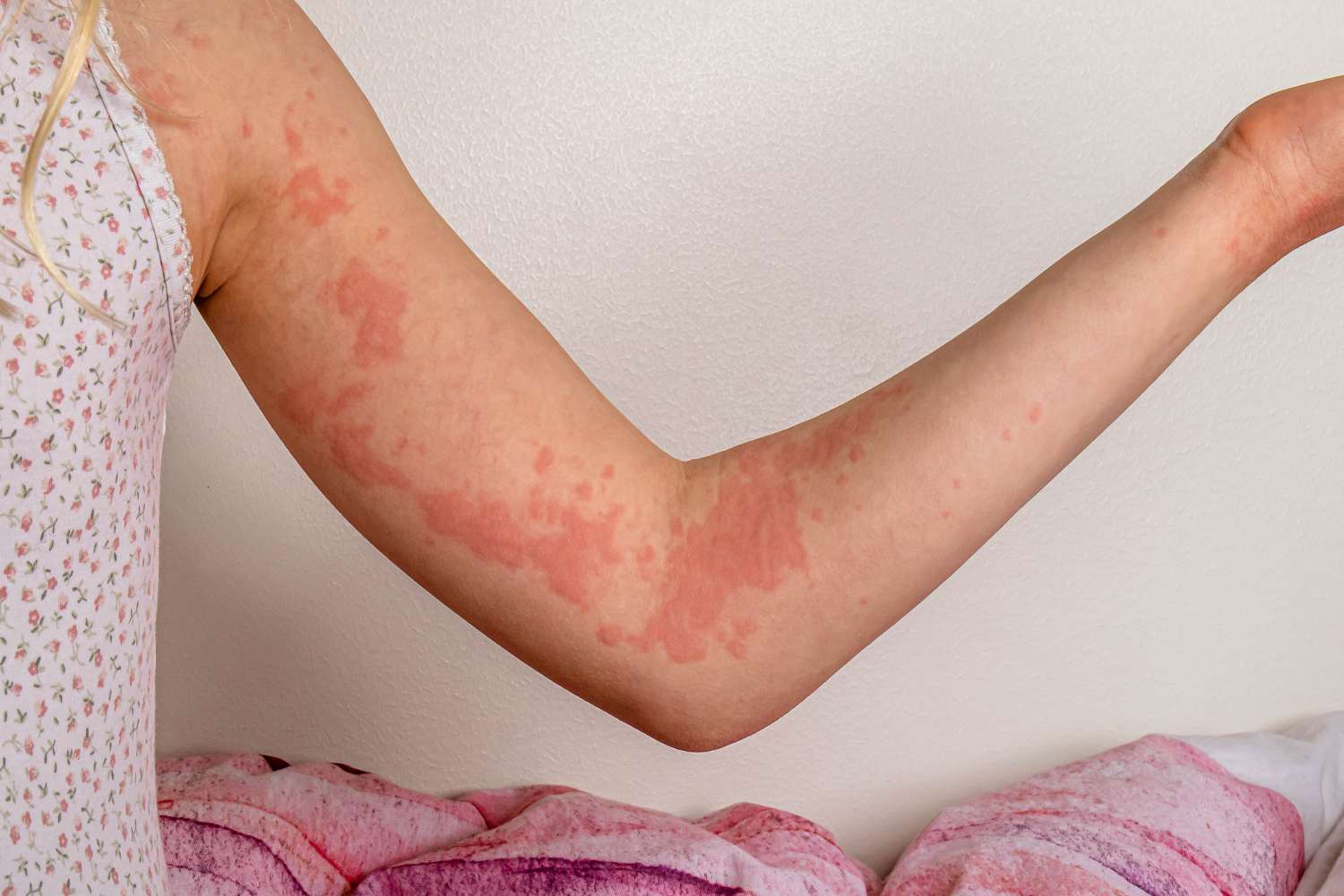
Hives (urticaria) are red, itchy bumps on the skin. You may develop hives for many reasons, including allergic reactions, but the cause may not always be known. Sometimes hives are long-lasting (chronic) and can come and go for months or years.
When hives are long-lasting without a known cause, it is called chronic idiopathic urticaria (CIU) or chronic spontaneous urticaria (CSU). About half of the people who experience CIU are believed to have hives related to an autoimmune disease (when the immune system attacks healthy cells).
Learn about hives related to autoimmune activity, symptoms, treatment, and more.
Eik Scott / Getty Images
Do Autoimmune Diseases Cause Chronic Hives?
The link between autoimmune diseases and chronic hives is not completely understood. It is thought that about half of people with chronic hives have an autoimmune connection. However, most of these individuals do not have another autoimmune diagnosis. Autoimmune hives are sometimes referred to as chronic autoimmune urticaria (CAU).
Symptoms
Autoimmune hives look like other types of hives, showing up as red, itchy bumps or welts on the skin. Other symptoms can include fatigue or symptoms related to autoimmune diseases. For example, people with autoimmune thyroid diseases may experience weight changes along with hives. If left untreated, these uncomfortable symptoms can persist for years and may lead to emotional difficulties.
Symptoms of Autoimmune Hives
Diagnosis
Many people with autoimmune hives do not show other signs of autoimmunity. If autoimmune hives are suspected, a blood test is done to check for thyroid disease, which is the autoimmune condition most commonly associated with autoimmune hives.
No definitive tests diagnose autoimmune hives. Research studies sometimes report the basophil histamine release assay (BHRA) and/or the autologous serum skin test (ASST). Most clinics do not perform these tests.
Basophil Histamine Release Assay
The basophil histamine release assay (BHRA) test measures the release of histamine, a chemical that causes hives. Even if the test is positive, it does not confirm that you have autoimmune hives. It is mainly used in research to better understand the causes of autoimmune hives.
Autologous Serum Skin Test
The autologous serum skin test (ASST) is another test used in research studies for autoimmune hives. It involves a scratch to the skin using a person’s own serum (from blood) and, like the BHRA, assesses histamine response.
Treatment
Hives can be treated with:
- Over-the-counter (OTC) medications
- Prescription medications
- Complementary and alternative medicine (CAM)
Many treatment options, such as antihistamine medications, are the same whether or not the hives are autoimmune-related. With autoimmune hives, treatments for the autoimmune condition can help treat the hives associated with it. For example, treatments for thyroid disease may be effective in helping to resolve autoimmune hives that occur with thyroid disease.
Over-the-Counter (OTC) Therapies
OTC products can treat hives, including chronic and autoimmune hives. The gold standard for initial treatment of chronic hives (autoimmune or not) is nonsedating antihistamines, like Allegra (fexofenadine) and Zyrtec (cetirizine).
Prescriptions
Prescription medications are often used to treat hives, including autoimmune hives. Xolair (omalizumab) is often prescribed for chronic hives, while Vistaril (hydroxyzine) is a sedating antihistamine sometimes prescribed in cases of severe hives that impair sleep. Corticosteroids may also be prescribed.
Complementary and Alternative Medicine (CAM)
Prescription and OTC medications are not the only treatment options for hives; CAM options can help. For example, stress can trigger autoimmune hives, so therapies and practices that promote relaxation and relieve stress can help prevent and relieve autoimmune hives.
Some CAM methods that may help include:
When to See a Healthcare Provider
While hives are generally not severe, it is important to see a healthcare provider if the condition:
- Continues to come back after going away
- Does not improve in a couple of days
- Includes fever, swelling, difficulty breathing, or other signs of anaphylaxis (life-threatening allergic reaction)
- Leads to worry or fear
- Spreads to other areas of the body
As with other chronic conditions, chronic hives can increase your risk of developing mental health issues, such as depression or anxiety. Speak with your healthcare provider or a mental health provider if you experience any mental health concerns.






:max_bytes(150000):strip_icc()/AshleyOlivine-e60b0f7c436248b1ad12bd7a0b8ddc98.jpg)








Leave a Reply