Key Takeaways
- Blood thinners prevent blood clots from forming or growing.
- The main side effect of blood thinners is a higher risk of bleeding.
Blood thinners is a common term for anticoagulation medications used to treat and prevent blood clots. They do not thin the blood but instead block certain clotting proteins.
Blood travels through blood vessels in a liquid form to bring oxygen and nutrients to tissues throughout the body. When blood clots form in the body, they block normal blood flow from reaching tissues and can cause tissue death, such as in heart attack, stroke, and pulmonary embolism.
While anticoagulation medications can be lifesaving, they carry a risk of bleeding. This article discusses the types of blood thinners, their medical uses, and side effects.
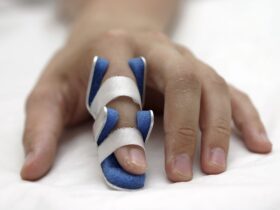
Daniel Grill / Getty Images
What Are Blood Thinners?
Blood thinners are anticoagulation medications that prevent and treat blood clots. Blood clots are semi-solid clumps made of red blood cells, platelets, fibrin (a type of protein), and other proteins.
Blood clotting is an extremely important function of the body that prevents bleeding. Without blood clotting, a small cut would cause serious, prolonged bleeding.
Thrombus vs. Embolus
Another word for blood clot is “thrombus,” but when a blood clot travels to another place in the body, it is known as “embolus.” For example, a “pulmonary embolism” is a blood clot that has traveled from the deep veins in the leg to the arteries in the lung.
Blood clots form through two important processes: the coagulation cascade and platelet activation. Blood thinners work by targeting steps in each of these processes.
In the coagulation cascade, damaged tissue sets off a cascade of events that activates several proteins in the blood, called clotting factors. These proteins are activated through a series of steps that, ultimately, activates fibrin. Fibrin is a protein formed during the clotting process that helps stop blood flow.
Another important part of blood clots is platelets. Damaged tissue activates platelets in the blood. Activated platelets attract other platelets, and they stick to each other to plug up the wound and stop the bleeding.
Red vs. White Clots
Blood clots rich in red blood cells and fibrins are known as “red clots,” whereas those rich in platelets, which are colorless, are referred to as “white clots.” Red clots are found in veins (like the leg veins), whereas white clots are found more in arteries (like the coronary arteries of the heart). The distinction of red vs. white is based on the color and composition of the clots, but all clots contain varying amounts of platelets, fibrin, and red blood cells.
Why Are Blood Thinners Prescribed?
Blood thinners are used to treat blood clots and prevent them from forming when they pose a risk to the body. Here are some specific conditions that may require blood thinners:
How Do Blood Thinners Work?
In general, anticoagulation medications work by blocking or inactivating parts of the system that form blood clots. These medications work by binding to proteins that are involved in either the coagulation cascade or to proteins on platelet surfaces.
Anticoagulant medications target the coagulation cascade, whereas antiplatelet medications target platelet activation. These medications can be oral pills or injections.
Types of Blood Thinners
Anticoagulants
Anticoagulant blood thinners target various proteins in the coagulation cascade. These medications are used for treating red clots, like deep vein thrombosis and pulmonary embolism, as well as preventing strokes in atrial fibrillation and mechanical heart valves.
Anticoagulants are also used during acute blood clotting in arteries (such as heart attacks, acute limb ischemia, and acute mesenteric ischemia). Examples of anticoagulants include:
- Warfarin
- Enoxaparin (low molecular weight heparin)
- Factor X inhibitors, such as Eliquis (apixaban) and Xarelto (rivaroxaban)
- Direct thrombin inhibitors, such as Acova (argatroban), Angiomax (bivalirudin), and Pradaxa (dabigatran)
- Tissue plasminogen activators such as Actilyse (alteplase), TNKase (tenecteplase), and Retavase (reteplase)
Antiplatelets
Antiplatelets are medications that target the activation and aggregation of platelets. They are commonly used in the treatment and prevention of stroke and heart attacks.
Antiplatelets are also used to protect stents placed in the heart’s coronary arteries and other arteries (such as carotid arteries of the neck and leg arteries in peripheral arterial disease).
Examples of antiplatelets include:
- Aspirin
- P2Y12 receptor blockers, such as Plavix (clopidogrel), Effient (prasugrel), and Brillinta (ticagrelor)
- Phosphodiesterase inhibitors, like dipyridamole and cilostazole
- GIIb/IIIa inhibitors, such as Reopro (abciximab), eptifibatide, and Aggrastat (tirofiban)
Side Effects
Unsurprisingly, the main side effect of blood thinners is bleeding. People who take blood thinners will notice that a cut or nick takes longer to stop bleeding and that they bruise more easily. But serious bleeding, such as bleeding in the gastrointestinal tract or brain, can occur. These bleeds can be life-threatening.
It is important to avoid contact sports or activities while taking anticoagulation.
Each specific drug has a list of side effects that can range from nausea, constipation, and headache, to shortness of breath and severe allergic reaction.
Natural Blood Thinners
Some foods and supplements are believed to have some blood thinning properties. However, they are not regulated by the Food and Drug Administration (FDA), and the concentration of active compounds in supplements is not consistent.
Always discuss any supplements you’re taking or considering with your healthcare provider, as they can interfere with other medications. Supplements should never be taken as a replacement for a prescribed blood-thinning medication.
The following have some evidence of blood-thinning properties:
- Cranberry
- Dong quai
- Fenugreek
- Feverfew
- Garlic
- Ginger
- Ginkgo
- Red Clover
- Turmeric
- White willow






:max_bytes(150000):strip_icc()/1000x1000pixjpg-f61393eb490a4aeba57e413c255b93af.jpg)











Leave a Reply