:max_bytes(150000):strip_icc():format(jpeg)/GettyImages-503814062-9c3b5714138142109cf6533ad59283c2.jpg)
Key Takeaways
- Chemotherapy can stop your periods temporarily or permanently, and the older you are, the more likely menopause will be permanent.
- Even if periods return after treatment, fertility is uncertain, and a fertility expert may be needed to assess your ability to conceive.
- Consider talking to a healthcare provider about fertility preservation before starting chemotherapy, such as freezing eggs or ovarian tissue.
Chemotherapy is a form of treatment for cancer. It is a group of medications used to kill cancer cells. Following chemotherapy, people with a uterus may experience changes in their libido (sex drive) and fertility.
The exact impact on fertility, which refers to a person’s ability to conceive through intercourse and carry the pregnancy to term, depends on your stage in life, menstrual history, hormone levels, the type of cancer and treatment, and the treatment doses. It can be hard to predict if someone is likely to be fertile after chemo.
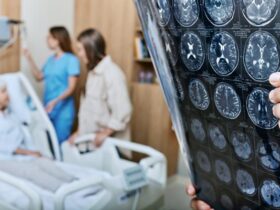
ShotShare / Getty Images
Chemotherapy and Ovarian Function
Chemotherapy can harm the female reproductive system, affecting both the reproductive organs and the hypothalamic-pituitary axis, which controls hormone regulation.
The hormones that are needed to release eggs each month, such as estrogen, and prepare the uterus for a possible pregnancy are made in the cells of the ovaries called oocytes.
Oocytes tend to divide quickly, so they are often affected by chemo, which kills fast-growing cells. This can lead to loss of those important hormones and can affect fertility. Sometimes a person will go into premature or early menopause after chemo.
Higher doses of these drugs are more likely to cause permanent fertility changes, and combinations of drugs can have greater side effects. The risk of permanent infertility is even higher when you are treated with both chemo and radiation therapy to the abdomen or pelvis.
What Is Radiation Therapy?
Radiation therapy (also called radiotherapy) is a cancer treatment that uses high doses of radiation to kill cancer cells and shrink tumors. At low doses, radiation is used in X-rays to view inside your body, as with X-rays of your teeth or broken bones.
Effect on Menstruation
Amenorrhea means not having a period. There are two types:
- Primary amenorrhea happens when someone hasn’t had a period by age 15, or two years after puberty begins, marked by breast development.
- Secondary amenorrhea is when someone misses periods for three months or has irregular periods for six months. Causes can include stress, low body weight, certain medications, excessive exercise, or eating disorders. It can also result from conditions like polycystic ovary syndrome (PCOS) or uterine scarring. Chemotherapy-induced amenorrhea is a form of secondary amenorrhea.
In one study of 1,043 women aged 20–35, all of whom got their initial cancer diagnosis at least two years before, 31.6% developed amenorrhea. Of those diagnosed with amenorrhea, 70% resumed their periods, and 90% did so within two years.
Effect on Fertility
Some factors increase the risk of infertility, while others may not affect fertility:
- Age: Younger people have more eggs in their ovaries, increasing the chance of preserving some fertility despite treatment damage. Those treated for cancer before age 35 have a better chance of becoming pregnant afterward.
- Puberty and menopause: People who had chemotherapy before puberty, or whose periods resume afterward, risk early menopause, which occurs when periods stop before age 40. This is also known as premature ovarian failure or primary ovarian insufficiency, and infertility happens because the ovaries stop producing necessary hormones.
It’s important to remember that even if periods start again after cancer treatment has stopped, fertility is still uncertain. A fertility expert may be needed to help you determine if you are fertile or learn how long the fertility window may last.
Many of the drugs used to treat cancer can harm the developing fetus during pregnancy. People usually are advised to use birth control to avoid getting pregnant during treatment.
Even if you think you can’t get pregnant, you should talk to your healthcare provider about options. It’s important to know what kind of birth control is best and safest for you to use. If you want to get pregnant, talk with your healthcare provider about how long you should wait after treatment ends.
Effect on Menopause
Chemotherapy-induced menopause is also known as medical menopause. Your periods may stop temporarily during chemotherapy, or they may stop for good. The older you are, the higher the risk that this menopause will be permanent.
The medication Cytoxan (cyclophosphamide) has been associated most closely with medical menopause, especially when used as part of a regimen called CMF: cyclophosphamide, methotrexate, and fluorouracil, or 5-FU. However, other chemotherapy combinations can also lead to medical menopause, such as:
- Cyclophosphamide, Adriamycin (doxorubicin), and Tolak (fluorouracil) topical cream
- Cyclophosphamide, Ellence (epirubicin), and fluorouracil
- Doxorubicin and cyclophosphamide
- Taxotere (Docetaxel), doxorubicin, and cyclophosphamide
Even if your periods continue during chemo, you may have menopausal symptoms. It’s similar to being in the state called perimenopause, which can start eight to 10 years before menopause. If you’re closer to natural menopause and were already having symptoms from that, you may find they get worse during chemotherapy.
The younger you are, the more likely it is that this menopause will only be temporary, and your periods will come back. Studies have found that up to 40% of women under 40 go into permanent menopause as a result of chemotherapy, while 70%–90% of women over 40 do.
In the case of CMF in particular, about half of premenopausal women stop their periods while on it. Among those in their 30s, about 25%–50% can expect to get their periods back.
Effect on Sex
Chemo has different side effects that can have an impact on libido (sexual desire), including fatigue, mouth soreness, neuropathy (nerve pain), nausea, decreased appetite, and pain. Anxiety or depression can also affect your sex life and leave little energy for sex. Sexual desire often returns during recovery or in between cycles of treatments.
People getting chemo also tend to be sensitive about their appearance. Hair loss, weight loss or gain, and skin changes might occur, depending on the type of chemo you’re getting.
Some chemo drugs that irritate the mouth may also affect all mucous membranes, which line the inside of your hollow organs, like the gastrointestinal tract and respiratory tract. This includes the lining of the vagina, which may become dry and inflamed.
You could also experience flare-ups (intensification of symptoms) of genital warts or herpes because of the immunosuppressive effect of chemotherapy drugs. Even if you have never had a flare, some people experience them for the first time while the body’s immune system is suppressed during chemo.
Types of Chemo Medications
Chemo drugs that have been linked to the risk of infertility in females include:
- Busulfan
- Carboplatin
- Carmustine
- Chlorambucil
- Cisplatin
- Cyclophosphamide
- Cytosine arabinoside
- Doxorubicin
- Ifosfamide
- Lomustine
- Melphalan
- Mitomycin-C
- Nitrogen mustard (mechlorethamine)
- Procarbazine
- Temozolomide
- Thiotepa
- Vinblastine
- Vincristine
Some chemo drugs have a lower risk of causing infertility in females. They include:
- 5-fluorouracil (5-FU)
- 6-mercaptopurine (6-MP)
- Bleomycin
- Cytarabine
- Dactinomycin
- Daunorubicin
- Epirubicin
- Etoposide (VP-16)
- Fludarabine
- Gemcitabine
- Idarubicin
- Methotrexate
Talk to your healthcare provider about the chemo drugs you will get and the fertility risks that come with them.
Chemotherapy and Birth Defect Link
There is a substantial risk of children being born with birth defects because of chemotherapy.
Particularly during the first trimester, chemotherapy greatly increases the risk of malformations. Even in the second and third trimesters, chemotherapy increases the risk of pregnancy complications and a compromised immune system in babies after birth.
It’s important to use birth control methods during treatment for chemotherapy, but avoid the pill. Chemotherapy can cause nausea, and vomiting may decrease the pill’s effectiveness.
Experts also recommend avoiding hormonal birth control containing estrogen. You may want to discuss progestin-only birth control with your healthcare provider.
The copper IUD (intrauterine device) is recommended for most females undergoing chemotherapy.
Making a Fertility Plan Before Chemotherapy
Fertility specialists, such as reproductive endocrinologists or reproductive immunologists, can help those undergoing chemotherapy develop a fertility plan. Your primary care physician, gynecologist (a doctor specializing in female reproductive health), or oncologist (a cancer specialist) may be able to refer you to an appropriate specialist.
Fertility preservation is an important consideration for people who wish to have children after chemotherapy. You may wish to discuss cryopreservation of embryos or oocytes with your healthcare provider before beginning chemotherapy.
A fast-freezing method called vitrification has demonstrated increased pregnancy success over older, slow-freezing methods. Freezing your eggs in your 20s and early 30s gives you the opportunity to use your young eggs later in life.
If you freeze eggs between treatments or shortly after treatments, it is recommended that they be screened for potential birth defects.
Another option is ovarian tissue cryopreservation, which involves removing the egg-producing portion of the ovary, called the ovarian cortex, before treatment, and then freezing and storing it. The tissue can be transplanted years later to make pregnancy possible. This preservation method is the recommended option if the chemotherapy treatment is urgent and cannot be delayed.
Coping with Hormonal Changes After Chemo
If you just finished chemo and are now going through menopause, it is likely that you are experiencing intense emotional and physical changes. Perhaps this is not what you were expecting at this phase in your life, and you could be feeling alone, uncomfortable, panicked, angry, or afraid.
There are some lifestyle changes that can help you work through these changes, including:
- Eat a healthy diet.
- Avoid alcohol and processed meats.
- Engage in light-to-moderate exercise regularly.
- Practice yoga, mindfulness, and meditation.
- Join a support group.
- Unwind and take your mind off stressful topics through a new hobby.
- Be patient and open to new approaches to sex and intimacy. Explore alternatives such as massage or cuddling.
- Get plenty of sleep.
















Leave a Reply