:max_bytes(150000):strip_icc():format(jpeg)/what-is-joint-effusion-189282_color1-5c1afda046e0fb000176973c.png)
Key Takeaways
-
Joint effusion is the buildup of fluid in or around a joint, causing swelling and pain.
-
It can be caused by infections, injuries, or arthritis and requires medical evaluation.
-
Treatment may include rest and applying ice; in severe cases, your healthcare provider may aspirate the joint to remove fluid.
Joint effusion, also known as a swollen joint, occurs when excess fluid builds up in a joint, often leading to symptoms like pain, swelling, and stiffness. It can result from various causes, including arthritis, injury, or infection; understanding the root cause is crucial for finding the right treatment.
Verywell / Emily Roberts
What Are the Signs of a Swollen Joint?
Regardless of what causes fluid to build up in a joint, the symptoms are generally similar. They can vary from mild to very severe.
Common symptoms of joint effusion include:
- Swelling, from mild puffiness to severe enlargement
- Pain, from a dull ache to sharp, stabbing pains that affect movement
- Redness and warmth, associated with inflammation or infection
Joint effusion can sometimes cause other symptoms, such as:
- Bruising and bleeding in the joint space, often from an injury
- Fever, chills, malaise, and weakness, when due to an infection
- A fluid-filled bump called a Baker’s cyst, from fluids that can’t be reabsorbed
- Loss of muscle strength, known as arthrogenic muscle inhibition, due to joint injury
When Is Joint Effusion an Emergency?
Seek emergency care if you experience:
- An injury such as a broken bone or torn ligament.
- Inability to move the joint
- Inability to put weight on the joint
- Joint that looks red or feels hot
- Numbness near the joint
- Fever
Why Do Joints Swell?
Joint effusion is a sign of joint inflammation and can be either infectious (septic) or noninfectious (aseptic).
Infectious joint effusion, known as septic arthritis, results from an infection. Noninfectious joint effusion can be caused by an injury or arthritis.
Click Play to Learn All About Joint Effusion
Infection
Septic arthritis typically results from a joint infection. This infection can stem from open wounds, like deep cuts, or an invasive procedure, like joint replacement.
A bloodstream infection, known as a systemic infection, can sometimes take hold in a joint, causing localized swelling and effusion. Joint effusion can also indicate Lyme arthritis, usually seen in the later stages of Lyme disease.
Signs of Septic Arthritis
When joint effusion is caused by an infection, the symptoms are typically intense and come on fast. The condition will usually be extremely painful, particularly with movement. Redness, warmth, and fever are also common.
Certain factors increase the risk of septic arthritis, including:
- Older age
- Diabetes
- Intravenous (IV) drug use
- Joint replacement
- Recent joint surgery
- Arthritis
- A compromised immune system (such as seen in people with HIV, organ transplant recipients, and people undergoing chemotherapy)
Injury
Injuries often cause joint effusion, especially in the knees. Car accidents, severe falls, or blunt impacts can lead to this condition.
Such injuries may involve bones, connective tissues like tendons and ligaments, or joint cartilage, like the meniscus. Repetitive joint stress can also cause effusion, often seen in work or sports-related overuse.
If the joint effusion is caused by a repetitive stress injury, other conditions like bursitis (inflammation of the fluid-filled sac that cushions a joint) and tenosynovitis (inflammation of the tendon sheath where a muscle attaches to a bone) are also common.
Pain, swelling, stiffness, and trouble extending or rotating the joint are other common symptoms of injury-related effusion.
Arthritis
Joint effusion is common in people with arthritis. The condition can be chronic (comes on slowly and is progressive) or acute (comes on fast and is severe).
There are two main categories of arthritis: osteoarthritis, a non-inflammatory form of arthritis that’s also called wear-and-tear arthritis, and autoimmune arthritis, a group of inflammatory autoimmune disorders in which the immune system attacks its own joints.
With osteoarthritis, joint effusion most commonly occurs when there is extensive joint damage. The knee is the joint that is most often affected.
Autoimmune arthritis may cause chronic joint effusion, but often occurs in acute episodes, known as flare-ups. Some autoimmune conditions that can cause joint effusion are:
- Rheumatoid arthritis. The most common form of autoimmune arthritis. It typically affects joints on both sides of the body.
- Gout. An autoimmune condition that causes swelling and pain, mainly in the big toe. The inflammation is caused by the formation of uric acid crystals in the joint space.
- Juvenile idiopathic arthritis. An autoimmune form of arthritis that develops in children.
- Psoriatic arthritis. An autoimmune form of arthritis that goes along with the chronic skin condition psoriasis.
How Is It Diagnosed?
Diagnosing joint effusion may involve a physical exam, imaging tests, and a lab evaluation of the fluid in your joint. Your healthcare provider will also discuss your medical history, current health, and symptoms.
Physical Examination
Your provider will examine your joint, touching (palpating) and moving (manipulating) it to assess severity and possible causes.
Here are some things your provider might notice during the exam:
- With arthritis, the lubricating tissue between the joints, or synovium, will often feel “boggy” or “mushy.” Except for gout, swelling is usually gradual.
- Joint infections tend to develop rapidly and cause severe pain and redness.
- A torn ligament or knee fracture will almost always cause swelling and the inability to bear weight on the joint.
Imaging Tests
After examining your knee, a provider may order imaging tests to see what’s causing the effusion. Each test has its pros and cons.
The imaging tests may include:
- Ultrasonography: This non-invasive imaging tool uses sound waves to help providers see bone and connective tissues. It can be used to confirm arthritis or inflammation of tendons or ligaments. However, it is less able to visualize soft tissues than other forms of imaging.
- X-rays and computed tomography (CT): Both of these imaging techniques use ionizing radiation to create images of bone and connective tissue. With CT, multiple X-ray images are combined into three-dimensional “slices” of a body part. CT and X-rays are often best for diagnosing bone fractures and arthritis.
- Magnetic resonance imaging (MRI): This imaging technique uses powerful magnetic fields and radio waves to create highly detailed images of soft tissue. MRI can be useful for seeing cartilage, ligaments, and other joint structures that the other tests cannot pick up as well.
Joint Fluid Analysis
Your provider might drain fluid from a swollen joint to reduce pressure and relieve pain. This can also reveal more about the effusion’s cause.
The fluid (synovial fluid) is removed with a needle and syringe during a procedure known as arthrocentesis. Synovial fluid is usually clear with the consistency of an egg white. Any changes in the appearance, texture, color, or composition of the fluid can provide clues about what might be causing the effusion in the joint.
A lab can analyze the fluid to determine if there are excess white blood cells (a sign of infection), uric acid crystals (a sign of gout), or other abnormalities that may narrow the possible causes.
Treatment Options for Swollen Joints
The standard first-line treatments for joint effusion include rest, ice application, immobilization, and a nonsteroidal anti-inflammatory drug (NSAID) like Advil (ibuprofen) or Aleve (naproxen).
If the swelling is severe, your provider may want to aspirate the joint to reduce pressure. They may give you a cortisone injection after the procedure to reduce inflammation and pain.
Infections can usually be treated with a 14-day course of a broad-spectrum oral antibiotic like ciprofloxacin. Serious infections like systemic gonorrhea or methicillin-resistant Staphylococcus aureus (MRSA) may require a two- and four-week course of intravenous (IV) antibiotics.
If you have rheumatoid arthritis or another form of autoimmune arthritis, medications can be prescribed to suppress the overactive immune response and relieve symptoms. Examples of these medications are immunosuppressive drugs like methotrexate or Humira (adalimumab).
Joint surgery (arthroplasty) is only used for serious joint injuries or to repair joints immobilized by arthritis. Severe cases may need a total joint replacement.
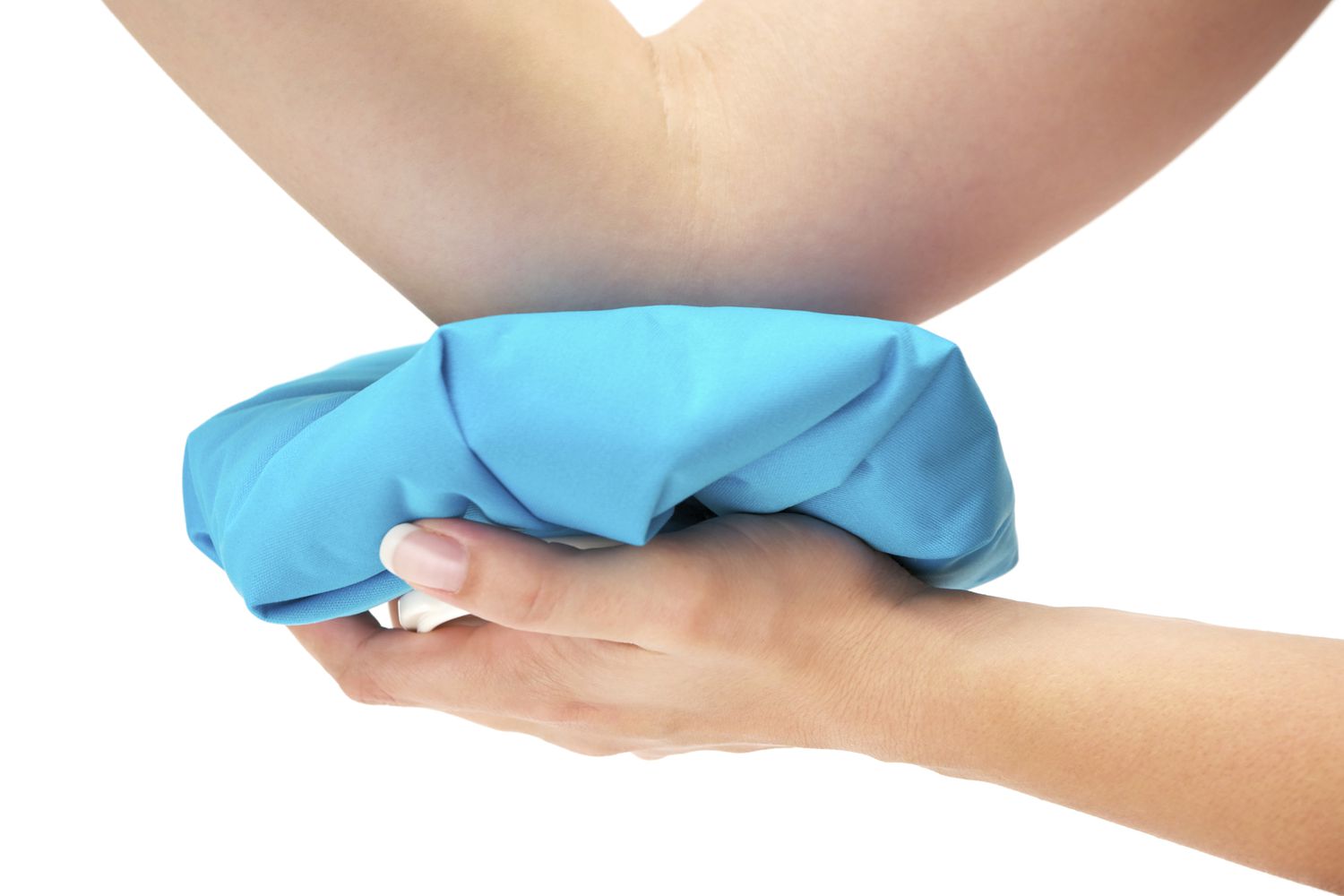
Home Remedies for Joint Effusion
While it is not a cure, you can ease joint swelling and pain at home by applying an ice pack for 15 to 20 minutes several times daily. A compression bandage can also help limit or reduce swelling. However, avoid wrapping the joint too tightly as doing so can cut off blood circulation.
How to Prevent It
While joint effusion cannot always be avoided, there are things you can do to significantly lower your risk of it occurring:
- Maintain a weight that supports your health: Losing weight and maintaining a weight that supports your health can reduce stress on the hips and lower extremities.
- Start a low-impact exercise plan: If you’re having pain in your knee, hip, or ankle, avoid high-impact activities like heavy weightlifting or deep squats.
- Use resistance training to strengthen joint muscles: Try using a leg extension machine for the knees or resistance band training for the shoulder and rotator cuff.
- Stretch. Perform gentle knee and shoulder stretches before exercise or throughout the day (especially if you’re sitting at a desk for long periods of time).
- Support your joints: Use elastic knee supports or an elbow brace during contact sports, hiking, and other vigorous physical activities.
- Don’t overdo it: Be mindful not to push yourself beyond your physical capabilities, especially as you get older. You may want to consider changing the types of sports you do to protect your joints (such as switching from running to swimming or cycling).
- Listen to your body: If you have sudden or persistent joint pain, don’t wait to see a provider for treatment.
When to See a Healthcare Provider
Seek emergency care if you have signs of infection or injury along with swelling. These symptoms include fever, redness around the joint, skin hot to the touch, and inability to move your joint or to put weight on it.
If you have a swollen joint without signs of an emergency, call your healthcare provider. They can have you come in for an appointment to find out what’s causing the joint swelling and make sure you get the right treatment. If they’re not sure, they might refer you to another provider who specializes in joints, like a rheumatologist or orthopedist.














Leave a Reply