:max_bytes(150000):strip_icc():format(jpeg)/what-to-know-about-reactive-hypoglycemia-1087744-ADD-FINAL-V2-816aeb42a8454caca819e5eb00f77d49.png)
Key Takeaways
- Reactive hypoglycemia is low blood sugar happening within four hours of eating.
- Symptoms of reactive hypoglycemia include a fast heartbeat, anxiety, sweating, and shaking.
- Eating high-carbohydrate meals can trigger reactive hypoglycemia.
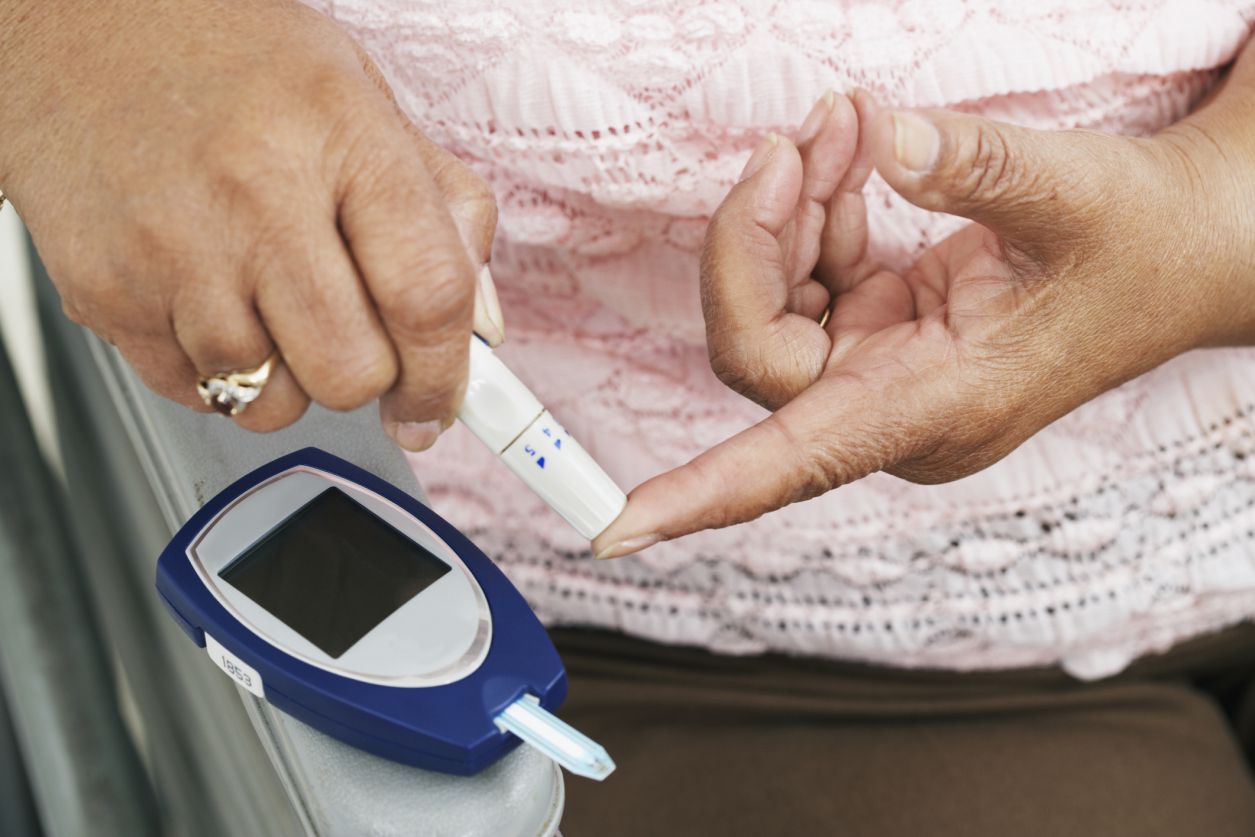
Reactive hypoglycemia happens when your blood sugar (blood glucose) drops to abnormally low levels after you eat. This “sugar crash” usually occurs within a few hours of eating. Why it happens is unclear, but it typically resolves quickly with a small amount of food or drink, like orange juice, or with glucose gel. It is also called postprandial hypoglycemia.
Reactive hypoglycemia can occur in people with or without diabetes. It can also occur after bariatric (weight loss) surgery or, rarely, due to insulinoma (endocrine tumor).
Illustration by Alex Dos Diaz for Verywell Health
Symptoms and Signs
“Hypoglycemia” means low blood sugar. Symptoms often happen when blood sugar drops below 70 milligrams per deciliter (mg/dL).
Common signs of reactive hypoglycemia include:
- Anxiety
- Shaking or tremors
- Heart palpitations
- Sweating
- Irritability
- Confusion
- Dizziness
- Hunger
- Nausea
Reactive hypoglycemia happens after eating and differs from hypoglycemia that occurs from fasting or when managing diabetes.
While symptoms are rarely life-threatening, they might indicate an underlying issue like Addison’s disease. If you experience severe symptoms, seek medical help immediately.
When to See a Healthcare Provider
Seek immediate medical attention if a severe drop in blood sugar cannot be reversed with glucose gel or a fast-acting food or drink. Severe symptoms may include:
- Pale skin
- Fatigue
- Weakness
- Blurry or double-vision
- Tingling in the lips, tongue, or cheeks
- Headaches
- Sleep disturbances
- Seizures
Notify your healthcare provider if you experience reactive hypoglycemia more often, even if symptoms aren’t severe.
Causes
Reactive hypoglycemia can affect people with or without diabetes. For those with diabetes, it may happen if too much insulin is taken before a meal.
For those without diabetes, factors like a family history may increase the risk of developing diabetes if experiencing reactive hypoglycemia.
Triggers include high-carbohydrate meals or snacks. High glycemic index foods cause insulin production to balance high blood sugar hyperglycemia). If the body doesn’t make enough glucagon—a hormone balancing insulin—blood sugar levels can drop.
Other health conditions causing reactive hypoglycemia include:
- Hyperinsulinemia: Insulin resistance may cause the pancreas to produce excess insulin, leading to low blood sugar after eating.
- Addison’s disease: This results in a deficiency of adrenal gland hormones, increasing insulin sensitivity.
- Insulinomas: Rare, non-cancerous pancreas tumors that cause excess insulin production, leading to low blood sugar. These usually cause fasting hypoglycemia but can occur after meals.
- Stress: Stress may affect blood sugar, causing an adrenaline rush that increases blood sugar temporarily. Stress may also lead to overeating, raising blood sugar levels.
- Bariatric surgery: Also called gastric bypass surgery, this treatment typically used for severe obesity can lead to reactive hypoglycemia as a complication. Food passes more quickly and changes how glucose is used. Some people can have similar responses due to early or late dumping syndromes caused by other digestive changes or surgeries.
- Delayed gastric emptying: Many people with diabetes have delayed gastric emptying, which can affect how the body responds to glucose.
- NIPHS: Non-insulinoma pancreatogenic hypoglycemia syndrome (NIPHS) is a rare condition that can lead to reactive hypoglycemia. It can occur after bariatric surgery, but that’s not always the cause.
- Genetic changes: Research has identified genetic mutations that lead to reactive hypoglycemia with other symptoms, including long QT syndrome (a cardiac condition).
- Certain cancers: The deficiency of certain digestive enzymes or hormones can be due to chronic conditions like pancreatic cancer. These endocrine problems interfere with the body’s ability to break down food. This, in turn, can reduce the amount of glucose available in the body.
Diagnosis
Reactive hypoglycemia can be diagnosed using an oral glucose tolerance test (OGTT) or a mixed meal tolerance test (MMTT).
The OGTT includes only glucose. The MMTT is performed by feeding the person a beverage rich in protein, carbohydrates, and fat (such as Ensure or Boost). Glucose and insulin levels are then assessed.
The healthcare provider will look for results, often called the Whipple’s Triad, that include:
- Symptoms known or likely to be caused by hypoglycemia
- Low plasma glucose measured at the time of the symptoms
- Relief of symptoms when glucose is raised to normal
Results from tests used to diagnose hypoglycemia also can help your healthcare provider to rule out other possible causes of the symptoms, including mental health concerns like anxiety.
Treatment
Treatment for reactive hypoglycemia will depend on the cause. In many cases, blood sugar can be corrected quickly and people don’t need medical treatment. However, if the symptoms are recurring, they may be the result of an underlying condition that needs treatment.
If you have an episode of reactive hypoglycemia, you can use food to help restore normal blood sugar levels.
This is accomplished with the “15-15 Rule,” which involves eating 15 grams of fast-acting carbohydrates and checking your blood sugar 15 minutes later to see if the levels have normalized. The American Diabetic Association recommends:
- Glucose tablets or a gel tube, administered per the directions
- 4 ounces of juice or regular soda
- 1 tablespoon of sugar, honey, or corn syrup
- Hard candies, jellybeans, or gumdrops
Once your symptoms have eased, have a snack if your next meal is more than an hour away to prevent your blood sugar from dropping again.
Sometimes, medication is prescribed to help treat reactive hypoglycemia. These medications may delay the digestion of carbohydrates or reduce insulin secretion. They include:
- Alpha-glucosidase inhibitors
- Calcium channel blockers
- Proglycem (diazoxide)
- Somatostatin analogues
These medications may have uncomfortable side effects, however, and may not work well for everyone.
For an underlying medical condition, the treatment will focus on resolving or managing the condition. This may include the surgical removal of an insulinoma or, in the case of NIPHS, the partial removal of the pancreas.
Prevention
Certain dietary and lifestyle changes may reduce the odds of a reactive hypoglycemia episode, even where the cause is not yet known. You can try:
- Adopting a diet with lean protein, whole grains, vegetables, fruits, and low-fat dairy
- Eating smaller meals more often
- Avoiding alcohol and sugary mixers on an empty stomach
- Getting more exercise
- Managing stress
- Avoiding eating large amounts of sugar or refined carbs at a time
If you have diabetes, it’s important to monitor your blood sugar regularly and keep your blood sugar levels under control.
Talk to your healthcare provider about your symptoms and lifestyle changes, as it’s possible that medication or other measures may be needed, too.












Leave a Reply