The efficacy of vaccination and previous infection in mediating protective humoral responses depends on the survival of long-lived plasma cells (LLPCs) in the bone marrow niche that sustain the systemic release of neutralizing antibodies. The lifespan of LLPCs is highly variable between individuals and in response to different vaccines and infections but the intrinsic and extrinsic factors that regulate LLPC survival are unclear. Zhu et al. report that intermittent fasting, which has been shown in other contexts to have beneficial effects on health and longevity, results in the eviction of LLPCs from their survival niche in the bone marrow and thus impairs humoral immunity.
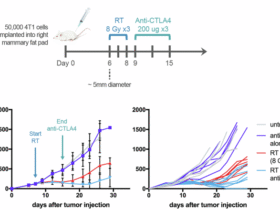
Furthermore, in vaccination models in which wild-type mice were immunized with NP-KLH, inactivated influenza vaccine or the SARS-CoV-2 vaccine Ad5-nCoV, mice that were fasted starting more than 8 weeks after vaccination — to analyse the effect on already generated antigen-specific LLPCs — had reduced antigen-specific IgG in serum and reduced antigen-specific LLPCs in bone marrow. Vaccinated mice that were fasted later had reduced protection against influenza virus challenge and reduced serum neutralization activity in a SARS-CoV-2 pseudovirus neutralization assay. In the context of natural infection with lymphocytic choriomeningitis virus (LCMV), mice subjected to ADF or prolonged fasting initiated more than 8 weeks after infection had reduced serum levels of anti-LCMV IgG. Thus, intermittent fasting impairs the maintenance of humoral memory by depleting antigen-specific LLPCs.















Leave a Reply