Bianconi, E. et al. An estimation of the number of cells in the human body. Ann. Hum. Biol. 40, 463–471 (2013).
Moras, M., Lefevre, S. D. & Ostuni, M. A. From erythroblasts to mature red blood cells: organelle clearance in mammals. Front. Physiol. 8, 1076 (2017).
de Back, D. Z., Kostova, E. B., van Kraaij, M., van den Berg, T. K. & van Bruggen, R. Of macrophages and red blood cells; a complex love story. Front. Physiol. 5, 9 (2014).
Anderson, H. L., Brodsky, I. E. & Mangalmurti, N. S. The evolving erythrocyte: red blood cells as modulators of innate immunity. J. Immunol. 201, 1343–1351 (2018).
Workenhe, S. T. et al. Infectious salmon anaemia virus replication and induction of alpha interferon in Atlantic salmon erythrocytes. Virol. J. 5, 36 (2008).
Elahi, S. New insight into an old concept: role of immature erythroid cells in immune pathogenesis of neonatal infection. Front. Immunol. 5, 376 (2014).
Sankaran, V. G. & Weiss, M. J. Anemia: progress in molecular mechanisms and therapies. Nat. Med. 21, 221–230 (2015).
Palis, J., Robertson, S., Kennedy, M., Wall, C. & Keller, G. Development of erythroid and myeloid progenitors in the yolk sac and embryo proper of the mouse. Development 126, 5073–5084 (1999).
Li, H. J. et al. Rate of progression through a continuum of transit-amplifying progenitor cell states regulates blood cell production. Dev. Cell 49, 118–129 (2019).
Velten, L. et al. Human haematopoietic stem cell lineage commitment is a continuous process. Nat. Cell Biol. 19, 271–281 (2017).
Tusi, B. K. et al. Population snapshots predict early haematopoietic and erythroid hierarchies. Nature 555, 54–60 (2018). This study represents a conceptual advance in stem cell biology by linking population-level transcriptomic snapshots to predictive fate modelling, thereby resolving early erythroid commitment and uncovering previously unappreciated lineage coupling and regulatory mechanisms.
Valent, P. et al. Normal and pathological erythropoiesis in adults: from gene regulation to targeted treatment concepts. Haematologica 103, 1593–1603 (2018).
Caulier, A. & Sankaran, V. G. Molecular and cellular mechanisms that regulate human erythropoiesis. Blood 140, 1451–1451 (2022).
Weiss, G., Ganz, T. & Goodnough, L. T. Anemia of inflammation. Blood 133, 40–50 (2019).
Nairz, M. et al. Erythropoietin contrastingly affects bacterial infection and experimental colitis by inhibiting nuclear factor-kB-inducible immune pathways. Immunity 34, 61–74 (2011).
Peng, B., Kong, G., Yang, C. & Ming, Y. Erythropoietin and its derivatives: from tissue protection to immune regulation. Cell Death Dis. 11, 79 (2020).
Camaschella, C., Pagani, A., Silvestri, L. & Nai, A. The mutual crosstalk between iron and erythropoiesis. Int. J. Hematol. 116, 182–191 (2022).
Jelkmann, W. Regulation of erythropoietin production. J. Physiol. 589, 1251–1258 (2011).
Taylor, C. T. & Scholz, C. C. The effect of HIF on metabolism and immunity. Nat. Rev. Nephrol. 18, 573–587 (2022).
Cheng, S. C. et al. mTOR- and HIF-1α-mediated aerobic glycolysis as metabolic basis for trained immunity. Science 345, 1250684 (2014).
Jacobs-Helber, S. M. et al. Tumor necrosis factor-α expressed constitutively in erythroid cells or induced by erythropoietin has negative and stimulatory roles in normal erythropoiesis and erythroleukemia. Blood 101, 524–531 (2003).
Han, Y. et al. Hemolysis-driven IFNα production impairs erythropoiesis by negatively regulating EPO signaling in sickle cell disease. Blood 143, 1018–1031 (2024).
de Bruin, A. M., Voermans, C. & Nolte, M. A. Impact of interferon-γ on hematopoiesis. Blood 124, 2479–2486 (2014).
Le Goff, S. et al. p53 activation during ribosome biogenesis regulates normal erythroid differentiation. Blood 137, 89–102 (2021).
Canny, S. P., Orozco, S. L., Thulin, N. K. & Hamerman, J. A. Immune mechanisms in inflammatory anemia. Annu. Rev. Immunol. 41, 405–429 (2023).
Klei, T. R., Meinderts, S. M., van den Berg, T. K. & van Bruggen, R. From the cradle to the grave: the role of macrophages in erythropoiesis and erythrophagocytosis. Front. Immunol. 8, 73 (2017).
Li, W. et al. Identification and transcriptome analysis of erythroblastic island macrophages. Blood 134, 480–491 (2019).
Chasis, J. A. & Mohandas, N. Erythroblastic islands: niches for erythropoiesis. Blood 112, 470–478 (2008).
Cao, W. et al. GM-CSF impairs erythropoiesis by disrupting erythroblastic island formation via macrophages. J. Transl. Med. 20, 11 (2022).
Buesche, G. et al. Impaired formation of erythroblastic islands is associated with erythroid failure and poor prognosis in a significant proportion of patients with myelodysplastic syndromes. Haematologica 101, e177–e181 (2016).
Ramos, P. et al. Macrophages support pathological erythropoiesis in polycythemia vera and β-thalassemia. Nat. Med. 19, 437–445 (2013).
Liao, C., Prabhu, K. S. & Paulson, R. F. Monocyte-derived macrophages expand the murine stress erythropoietic niche during the recovery from anemia. Blood 132, 2580–2593 (2018).
Long, H. et al. Tumor-induced erythroid precursor-differentiated myeloid cells mediate immunosuppression and curtail anti-PD-1/PD-L1 treatment efficacy. Cancer Cell 40, 674–693.e7 (2022).
Elahi, S. & Mashhouri, S. Immunological consequences of extramedullary erythropoiesis: immunoregulatory functions of CD71+ erythroid cells. Haematologica 105, 1478–1483 (2020).
Mitasov, A. V., Tsyrlova, I. G., Kiselev, S. V. & Kozlov, V. V. Species-nonspecific action of soluble immunosuppressive factor produced by murine immature erythroid cells. Ann. N. Y. Acad. Sci. 628, 399–409 (1991).
Seledtsova, G. V. et al. Erythroid cells in immunoregulation: characterization of a novel suppressor factor. Immunol. Lett. 93, 171–178 (2004).
Elahi, S. et al. Immunosuppressive CD71+ erythroid cells compromise neonatal host defence against infection. Nature 504, 158–162 (2013). This study identifies CD71⁺ erythroid cells as a developmentally enriched immunosuppressive population in neonates, redefining susceptibility to early-life infection as an actively regulated process that balances host defense with tolerance to postnatal microbial colonization.
Elahi, S. Neglected cells: immunomodulatory roles of CD71+ erythroid cells. Trends Immunol. 40, 181–185 (2019).
Elahi, S. et al. Galectin-3 regulates erythropoiesis and enhances the immunoregulatory properties of CD71+ erythroid cells across developmental stages. J. Immunol. 214, 1202–1218 (2025).
Elahi, S. et al. CD71+ erythroid cells in human neonates exhibit immunosuppressive properties and compromise immune response against systemic infection in neonatal mice. Front. Immunol. 11, 597433 (2020).
Delyea, C. et al. CD71+ Erythroid suppressor cells promote fetomaternal tolerance through arginase-2 and PDL-1. J. Immunol. 200, 4044–4058 (2018).
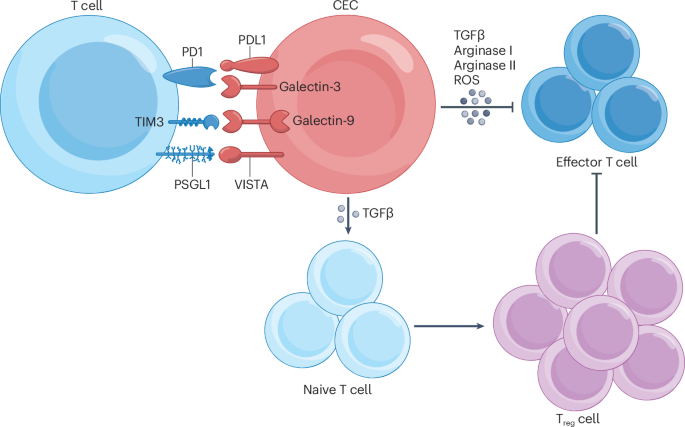
Shahbaz, S. et al. CD71+VISTA+ erythroid cells promote the development and function of regulatory T cells through TGF-β. PLoS Biol. 16, e2006649 (2018).
Grzywa, T. M. et al. Potent but transient immunosuppression of T-cells is a general feature of CD71+ erythroid cells. Commun. Biol. 4, 1384 (2021).
Gozzelino, R., Jeney, V. & Soares, M. P. Mechanisms of cell protection by heme oxygenase-1. Annu. Rev. Pharmacol. Toxicol. 50, 323–354 (2010).
Elahi, S. Neonatal and children’s immune system and COVID-19: biased immune tolerance versus resistance strategy. J. Immunol. 205, 1990–1997 (2020).
Adkins, B. Development of neonatal Th1/Th2 function. Int. Rev. Immunol. 19, 157–171 (2000).
Adkins, B., Leclerc, C. & Marshall-Clarke, S. Neonatal adaptive immunity comes of age. Nat. Rev. Immunol. 4, 553–564 (2004).
Kollmann, T. R., Kampmann, B., Mazmanian, S. K., Marchant, A. & Levy, O. Protecting the newborn and young infant from infectious diseases: lessons from immune ontogeny. Immunity 46, 350–363 (2017).
Behnke, J. M., Barnard, C. J. & Wakelin, D. Understanding chronic nematode infections: evolutionary considerations, current hypotheses and the way forward. Int. J. Parasitol. 22, 861–907 (1992).
Read, A. F., Graham, A. L. & Raberg, L. Animal defenses against infectious agents: is damage control more important than pathogen control? PLoS Biol. 6, 2638–2641 (2008).
Medzhitov, R., Schneider, D. S. & Soares, M. P. Disease tolerance as a defense strategy. Science 335, 936–941 (2012).
Hornik, C. P. et al. Use of the complete blood cell count in early-onset neonatal sepsis. Pediatr. Infect. Dis. J. 31, 799–802 (2012).
Zhao, J. et al. Hyper innate responses in neonates lead to increased morbidity and mortality after infection. Proc. Natl Acad. Sci. USA 105, 7528–7533 (2008).
Dunsmore, G. et al. Erythroid suppressor cells compromise neonatal immune response against Bordetella pertussis. J. Immunol. 199, 2081–2095 (2017).
Dunsmore, G. et al. Lower abundance and impaired function of CD71+ erythroid cells in inflammatory bowel disease patients during pregnancy. J. Crohns Colitis 13, 230–244 (2019).
Dunsmore, G. et al. Mode of delivery by an ulcerative colitis mother in a case of twins: immunological differences in cord blood and placenta. World J. Gastroenterol. 24, 4787–4797 (2018).
Cho, H., Oh, J. H., Kim, Y. & Jeong, D. C. The profile of CD71+ erythroid cells in Korean children: a pilot study. Pediatr. Allergy Immunol. Pulmonol. 38, 78–81 (2025).
Namdar, A. et al. CD71+ erythroid suppressor cells impair adaptive immunity against Bordetella pertussis. Sci. Rep. 7, 7728 (2017).
Yang, L. et al. Regulation of bile duct epithelial injury by hepatic CD71+ erythroid cells. JCI Insight 5, e135751 (2020).
Thaiss, C. A., Zmora, N., Levy, M. & Elinav, E. The microbiome and innate immunity. Nature 535, 65–74 (2016).
Rakoff-Nahoum, S., Paglino, J., Eslami-Varzaneh, F., Edberg, S. & Medzhitov, R. Recognition of commensal microflora by toll-like receptors is required for intestinal homeostasis. Cell 118, 229–241 (2004).
Slack, E. et al. Innate and adaptive immunity cooperate flexibly to maintain host–microbiota mutualism. Science 325, 617–620 (2009).
Koleva, P. et al. CD71+ erythroid cells promote intestinal symbiotic microbial communities in pregnancy and neonatal period. Microbiome 12, 142 (2024). This study identifies gut-resident CD71⁺ erythroid cells as key regulators of microbial colonization and immune homeostasis during early life.
Warner, B. B. et al. Gut bacteria dysbiosis and necrotising enterocolitis in very low birthweight infants: a prospective case-control study. Lancet 387, 1928–1936 (2016).
Rowe, J. H., Ertelt, J. M., Xin, L. J. & Way, S. S. Pregnancy imprints regulatory memory that sustains anergy to fetal antigen. Nature 490, 102–U119 (2012).
Chabtini, L. et al. TIM-3 regulates innate immune cells to induce fetomaternal tolerance. J. Immunol. 190, 88–96 (2013).
Guleria, I. et al. A critical role for the programmed death ligand 1 in fetomaternal tolerance. J. Exp. Med. 202, 231–237 (2005).
Parasar, P., Guru, N. & Nayak, N. R. Contribution of macrophages to fetomaternal immunological tolerance. Hum. Immunol. 82, 325–331 (2021).
Crux, N. B. & Elahi, S. Human leukocyte antigen (HLA) and immune regulation: how do classical and non-classical HLA alleles modulate immune response to human immunodeficiency virus and hepatitis C virus infections? Front. Immunol. 8, 832 (2017).
McGovern, N. et al. Human fetal dendritic cells promote prenatal T-cell immune suppression through arginase-2. Nature 546, 662–666 (2017).
Dulmovits, B. M. et al. Inhibition of human erythropoiesis during inflammation is mediated by high mobility group box protein 1 (HMGB1) through decreased commitment of hematopoietic stem cells to the erythroid lineage and by increased apoptosis of terminally differentiating erythroblasts. Blood 128, 702 (2016).
Gomez-Lopez, N. et al. Umbilical cord CD71+ erythroid cells are reduced in neonates born to women in spontaneous preterm labor. Am. J. Reprod. Immunol. 76, 280–284 (2016).
Fraenkel, P. G. Anemia of Inflammation: a review. Med. Clin. North Am. 101, 285–296 (2017).
Weiss, G. & Goodnough, L. T. Anemia of chronic disease. N. Engl. J. Med. 352, 1011–1023 (2005).
Zhao, L. et al. Late-stage tumors induce anemia and immunosuppressive extramedullary erythroid progenitor cells. Nat. Med. 24, 1536–1544 (2018). This study shows CD45⁺ erythroid progenitor cells as a dominant immunosuppressive population in advanced cancer.
Shahbaz, S. et al. Erythroid precursors and progenitors suppress adaptive immunity and get invaded by SARS-CoV-2. Stem Cell Rep. 16, 1165–1181 (2021). This study highlights erythroid progenitors as key immunoregulatory and virus-permissive cells in COVID-19, with dexamethasone-mediated modulation of ACE2/TMPRSS2 providing a mechanistic rationale for targeted intervention.
Huerga Encabo, H. et al. Human erythroid progenitors are directly infected by SARS-CoV-2: implications for emerging erythropoiesis in severe COVID-19 patients. Stem Cell Rep. 16, 428–436 (2021). This study implicates erythroid progenitors as unrecognized target of SARS-CoV-2, providing mechanistic insight into anemia, hypoxia and systemic inflammatory sequelae in severe COVID-19.
Kronstein-Wiedemann, R. et al. SARS-CoV-2 infects red blood cell progenitors and dysregulates hemoglobin and iron metabolism. Stem Cell Rev. Rep. 18, 1809–1821 (2022).
Elahi, S. Hematopoietic responses to SARS-CoV-2 infection. Cell. Mol. Life Sci. 79, 187 (2022).
Saito, S. et al. Differential impact of SARS-CoV-2 isolates, namely, the Wuhan strain, Delta, and Omicron variants on erythropoiesis. Microbiol. Spectr. 10, e0173022 (2022).
Shahbaz, S. et al. Analysis of SARS-CoV-2 isolates, namely the Wuhan strain, Delta variant, and Omicron variant, identifies differential immune profiles. Microbiol. Spectr. 11, e0125623 (2023).
Gabernet, G. et al. A multi-omics recovery factor predicts long COVID in the IMPACC study. J. Clin. Invest. 135, e193698 (2025).
Saito, S. et al. Diverse immunological dysregulation, chronic inflammation, and impaired erythropoiesis in long COVID patients with chronic fatigue syndrome. J. Autoimmun. 147, 103267 (2024).
Shahbaz, S. et al. Integrated immune, hormonal, and transcriptomic profiling reveals sex-specific dysregulation in long COVID patients with ME/CFS. Cell Rep. Med. 6, 102449 (2025).
Elahi, S., Rezaeifar, M., Osman, M. & Shahbaz, S. Exploring the role of galectin-9 and artemin as biomarkers in long COVID with chronic fatigue syndrome: links to inflammation and cognitive function. Front. Immunol. 15, 1443363 (2024).
Honma, Y. et al. Artemin is a vascular-derived neurotropic factor for developing sympathetic neurons. Neuron 35, 267–282 (2002).
Morgan, M. et al. Artemin sensitizes nociceptors that innervate the osteoarthritic joint to produce pain. Osteoarthr. Cartil. 31, 1342–1352 (2023).
He, W. et al. Duffy antigen receptor for chemokines mediates trans-infection of HIV-1 from red blood cells to target cells and affects HIV-AIDS susceptibility. Cell Host Microbe 4, 52–62 (2008).
Hess, C. et al. Association of a pool of HIV-1 with erythrocytes in vivo: a cohort study. Lancet 359, 2230–2234 (2002).
Namdar, A. et al. CD71+ erythroid cells exacerbate HIV-1 susceptibility, mediate trans-infection, and harbor infective viral particles. mBio 10, e02767-19 (2019). This study reveals that CD71⁺ erythroid cells act as immunoregulatory and HIV-permissive reservoirs, facilitating viral replication and trans-infection of CD4⁺ T cells.
Mhashilkar, A. M., Biswas, D. K., LaVecchio, J., Pardee, A. B. & Marasco, W. A. Inhibition of human immunodeficiency virus type 1 replication in vitro by a novel combination of anti-Tat single-chain intrabodies and NF-kB antagonists. J. Virol. 71, 6486–6494 (1997).
Bertram, K. M. et al. Identification of HIV transmitting CD11c+ human epidermal dendritic cells. Nat. Commun. 10, 2759 (2019).
Harman, A. N. et al. HIV-1-infected dendritic cells show 2 phases of gene expression changes, with lysosomal enzyme activity decreased during the second phase. Blood 114, 85–94 (2009).
Bozorgmehr, N. et al. CD71+ erythroid cells suppress T-cell effector functions and predict immunotherapy outcomes in patients with virus-associated solid tumors. J. Immunother. Cancer 11, e006595 (2023).
Wu, Z. Z. et al. Erythroid progenitor cell-mediated spleen-tumor interaction deteriorates cancer immunity. Proc. Natl Acad. Sci. USA 122, e2417473122 (2025).
Hu, T. H. et al. HDGF stimulates liver tumorigenesis by enhancing reactive oxygen species generation in mitochondria. J. Biol. Chem. 299, 105335 (2023).
Morad, G., Helmink, B. A., Sharma, P. & Wargo, J. A. Hallmarks of response, resistance, and toxicity to immune checkpoint blockade. Cell 185, 576 (2022).
Bozorgmehr, N., Syed, H., Mashhouri, S., Walker, J. & Elahi, S. Transcriptomic profiling of peripheral blood cells in HPV-associated carcinoma patients receiving combined valproic acid and avelumab. Mol. Oncol. 18, 1209–1230 (2023).
Hou, Y. Z. et al. Radiotherapy and immunotherapy converge on elimination of tumor-promoting erythroid progenitor cells through adaptive immunity. Sci. Transl. Med. 13, eabb0130 (2021).
Banerjee, A. et al. ARTEMIN synergizes with TWIST1 to promote metastasis and poor survival outcome in patients with ER negative mammary carcinoma. Breast Cancer Res. 13, R112 (2011).
Ceyhan, G. O. et al. The neurotrophic factor artemin promotes pancreatic cancer invasion. Ann. Surg. 244, 274–281 (2006).
Han, Y. et al. Tumor-induced generation of splenic erythroblast-like Ter-cells promotes tumor progression. Cell 173, 634–648.e12 (2018).
Chen, J. et al. Intratumoral CD45+CD71+ erythroid cells induce immune tolerance and predict tumor recurrence in hepatocellular carcinoma. Cancer Lett. 499, 85–98 (2021).
Wang, Y. et al. Intratumoral erythroblastic islands restrain anti-tumor immunity in hepatoblastoma. Cell Rep. Med. 4, 101044 (2023).
Rahmati, A. B. S. & Elahi, S. Galectin-9 promotes natural killer cells activity via interaction with CD44. Front. Immunol. 14, 1131379 (2023).
Torti, S. V., Tesfay, L. & Torti, F. M. Iron and cancer. Adv. Exp. Med. Biol. 1480, 271–289 (2025).
Frost, J. N. & Drakesmith, H. Iron and the immune system. Nat. Rev. Immunol. 25, 885–899 (2025).
Haschka, D., Hoffmann, A. & Weiss, G. Iron in immune cell function and host defense. Semin. Cell Dev. Biol. 115, 27–36 (2021).
Humar, R., Schaer, D. J. & Vallelian, F. Erythrophagocytes in hemolytic anemia, wound healing, and cancer. Trends Mol. Med. 28, 906–915 (2022).
Nakahira, K. et al. Circulating mitochondrial DNA in patients in the ICU as a marker of mortality: derivation and validation. PLoS Med. 10, e1001577 (2013).
Lam, L. K. M. et al. DNA binding to TLR9 expressed by red blood cells promotes innate immune activation and anemia. Sci. Transl. Med. 13, eabj1008 (2021). This work positions RBCs as central mediators of inflammation in sepsis and COVID-19, linking nucleic acid sensing to anaemia and disease severity.
Hotz, M. J. et al. Red blood cells homeostatically bind mitochondrial DNA through TLR9 to maintain quiescence and to prevent lung injury. Am. J. Resp. Crit. Care 197, 470–480 (2018).
Lam, L. K. M. et al. Red blood cells capture and deliver bacterial DNA to drive host responses during polymicrobial sepsis. J. Clin. Invest. 135, e182127 (2024).
Yi, T. S. et al. Splenic dendritic cells survey red blood cells for missing self-CD47 to trigger adaptive immune responses. Immunity 43, 764–775 (2015).
Caielli, S. et al. Erythroid mitochondrial retention triggers myeloid-dependent type I interferon in human SLE. Cell 184, 4464–4479.e19 (2021). This study identifies erythropoiesis as a previously unappreciated regulator of systemic autoimmunity.
Thompson, J. C. et al. Red blood cells function as reservoirs of tumor DNA. Am. J. Physiol. Lung Cell. Mol. Physiol. 326, L646–L650 (2024).
Metthew Lam, L. K. et al. Human red blood cells express the RNA sensor TLR7. Sci. Rep. 14, 15789 (2024).
Kim, H. et al. Functional roles for C5a and C5aR but not C5L2 in the pathogenesis of human and experimental cerebral malaria. Infect. Immun. 82, 371–379 (2014).
Darbonne, W. C. et al. Red blood cells are a sink for interleukin 8, a leukocyte chemotaxin. J. Clin. Invest. 88, 1362–1369 (1991).
Fukuma, N. et al. A role of the Duffy antigen for the maintenance of plasma chemokine concentrations. Biochem. Biophys. Res. Commun. 303, 137–139 (2003).
Minasyan, H. Oxycytosis and the role of triboelectricity and oxidation in bacteria clearing from the bloodstream. Eur. J. Microbiol. Immunol. 11, 23–28 (2021).
Edberg, J. C., Wright, E. & Taylor, R. P. Quantitative analyses of the binding of soluble complement-fixing antibody/dsDNA immune complexes to CR1 on human red blood cells. J. Immunol. 139, 3739–3747 (1987).
Minasyan, H. Mechanisms and pathways for the clearance of bacteria from blood circulation in health and disease. Pathophysiology 23, 61–66 (2016).
Mak, P., Wojcik, K., Silberring, J. & Dubin, A. Antimicrobial peptides derived from heme-containing proteins: hemocidins. Antonie Van Leeuwenhoek 77, 197–207 (2000).
Mak, P., Wojcik, K., Wicherek, L., Suder, P. & Dubin, A. Antibacterial hemoglobin peptides in human menstrual blood. Peptides 25, 1839–1847 (2004).
Mak, P., Szewczyk, A., Mickowska, B., Kicinska, A. & Dubin, A. Effect of antimicrobial apomyoglobin 56-131 peptide on liposomes and planar lipid bilayer membrane. Int. J. Antimicrob. Agents 17, 137–142 (2001).
Coates, C. J. & Decker, H. Immunological properties of oxygen-transport proteins: hemoglobin, hemocyanin and hemerythrin. Cell. Mol. Life Sci. 74, 293–317 (2017).
Chiabrando, D., Vinchi, F., Fiorito, V., Mercurio, S. & Tolosano, E. Heme in pathophysiology: a matter of scavenging, metabolism and trafficking across cell membranes. Front. Pharmacol. 5, 61 (2014).
Otterbein, L. E. et al. Carbon monoxide has anti-inflammatory effects involving the mitogen-activated protein kinase pathway. Nat. Med. 6, 422–428 (2000).
Dutra, F. F. & Bozza, M. T. Heme on innate immunity and inflammation. Front. Pharmacol. 5, 115 (2014).
Belcher, J. D. et al. Heme oxygenase-1 is a modulator of inflammation and vaso-occlusion in transgenic sickle mice. J. Clin. Invest. 116, 808–816 (2006).
Jentho, E. et al. Trained innate immunity, long-lasting epigenetic modulation, and skewed myelopoiesis by heme. Proc. Natl Acad. Sci. USA 118, e2102698118 (2021).
Chen, G. Y. & Nunez, G. Sterile inflammation: sensing and reacting to damage. Nat. Rev. Immunol. 10, 826–837 (2010).
Soares, M. P., Brouard, S., Smith, R. N. & Bach, F. H. Heme oxygenase-1, a protective gene that prevents the rejection of transplanted organs. Immunol. Rev. 184, 275–285 (2001).
Gupta, P. et al. Heme attenuates T cell exhaustion and drives effector function: implications for immune and adoptive T cell therapy. Blood 142, 6807 (2023).
Lennon, C. S., Cao, H., Hall, A. M., Vickers, M. A. & Barker, R. N. The red blood cell as a novel regulator of human B-cell activation. Immunology 163, 436–447 (2021).
Jin, L., McLean, P. A., Neel, B. G. & Wortis, H. H. Sialic acid binding domains of CD22 are required for negative regulation of B cell receptor signaling. J. Exp. Med. 195, 1199–1205 (2002).
Bozorgmehr, N. et al. Expanded antigen-experienced CD160+CD8+ effector T cells exhibit impaired effector functions in chronic lymphocytic leukemia. J. Immunother. Cancer 9, e002189 (2021).
Melder, R. J., Yuan, J., Munn, L. L. & Jain, R. K. Erythrocytes enhance lymphocyte rolling and arrest. Microvasc. Res. 59, 316–322 (2000).
Fonseca, A. M., Porto, G., Uchida, K. & Arosa, F. A. Red blood cells inhibit activation-induced cell death and oxidative stress in human peripheral blood T lymphocytes. Blood 97, 3152–3160 (2001).
Profumo, E. et al. Redox imbalance of red blood cells impacts T lymphocyte homeostasis: implication in carotid atherosclerosis. Thromb. Haemost. 106, 1117–1126 (2011).
Bernard, A. et al. Packed red blood cells suppress T-cell proliferation through a process involving cell–cell contact. J. Trauma 69, 320–327 (2010).
Baumgartner, J. M., Silliman, C. C., Moore, E. E., Banerjee, A. & McCarter, M. D. Stored red blood cell transfusion induces regulatory T cells. J. Am. Coll. Surg. 208, 110–119 (2009).
Richardson, J. D., Meredith, J. W. & Bernard, A. C. Intraoperative transfusion of 1 U to 2 U packed red blood cells is associated with increased 30-day mortality, surgical-site infection, pneumonia, and sepsis in general surgery patients discussion. J. Am. Coll. Surg. 208, 938–939 (2009).
Buttari, B., Profumo, E. & Riganò, R. Crosstalk between red blood cells and the immune system and its impact on atherosclerosis. Biomed. Res. Int. 2015, 616834 (2015).
Schiller, M. et al. Induction of type I IFN is a physiological immune reaction to apoptotic cell-derived membrane microparticles. J. Immunol. 189, 1747–1756 (2012).
Aoshiba, K., Nakajima, Y., Yasui, S., Tamaoki, J. & Nagai, A. Red blood cells inhibit apoptosis of human neutrophils. Blood 93, 4006–4010 (1999).
Meinderts, S. M. et al. Neutrophils acquire antigen-presenting cell features after phagocytosis of IgG-opsonized erythrocytes. Blood Adv. 3, 1761–1773 (2019).
Lizcano, A. et al. Erythrocyte sialoglycoproteins engage Siglec-9 on neutrophils to suppress activation. Blood 129, 3100–3110 (2017).
Motamedi, M., Xu, L. & Elahi, S. Correlation of transferrin receptor (CD71) with Ki67 expression on stimulated human and mouse T cells: the kinetics of expression of T cell activation markers. J. Immunol. Methods 437, 43–52 (2016).
Platzbecker, U. et al. Long-term utilization and benefit of luspatercept in transfusion-dependent, erythropoiesis-stimulating agent-refractory or -intolerant patients with lower-risk myelodysplastic syndromes with ring sideroblasts. Leukemia 37, 2314–2318 (2023).
Chen, L. et al. Dynamic changes in murine erythropoiesis from birth to adulthood: implications for the study of murine models of anemia. Blood Adv. 5, 16–25 (2021).
Thomas, T. et al. Evidence of structural protein damage and membrane lipid remodeling in red blood cells from COVID-19 patients. J. Proteome Res. 19, 4455–4469 (2020).
Kuhn, V. et al. Red blood cell function and dysfunction: redox regulation, nitric oxide metabolism, anemia. Antioxid. Redox Signal. 26, 718–742 (2017).
Johnson, R. M., Goyette, G. Jr., Ravindranath, Y. & Ho, Y. S. Hemoglobin autoxidation and regulation of endogenous H2O2 levels in erythrocytes. Free Radic. Biol. Med. 39, 1407–1417 (2005).
Low, F. M., Hampton, M. B. & Winterbourn, C. C. Peroxiredoxin 2 and peroxide metabolism in the erythrocyte. Antioxid. Redox Signal. 10, 1621–1630 (2008).
Obeagu, E. I., Igwe, M. C. & Obeagu, G. U. Oxidative stress’s impact on red blood cells: unveiling implications for health and disease. Medicine 103, e37360 (2024).
Rifkind, J. M., Mohanty, J. G. & Nagababu, E. The pathophysiology of extracellular hemoglobin associated with enhanced oxidative reactions. Front. Physiol. 5, 500 (2014).
Donadee, C. et al. Nitric oxide scavenging by red blood cell microparticles and cell-free hemoglobin as a mechanism for the red cell storage lesion. Circulation 124, 465–U294 (2011).
Pernow, J., Mahdi, A., Yang, J. & Zhou, Z. Red blood cell dysfunction: a new player in cardiovascular disease. Cardiovasc. Res. 115, 1596–1605 (2019).
Lee, S. K. et al. Complement receptor 1 is the human erythrocyte receptor for erythrocyte binding protein. Proc. Natl Acad. Sci. USA 121, e2316304121 (2024).
McCullough, J. RBCs as targets of infection. Hematol. Am Soc. Hematol. Educ. Program 2014, 404–409 (2014).
Ukidve, A. et al. Erythrocyte-driven immunization via biomimicry of their natural antigen-presenting function. Proc. Natl Acad. Sci. USA 117, 17727–17736 (2020).
Zhao, Z. et al. Systemic tumour suppression via the preferential accumulation of erythrocyte-anchored chemokine-encapsulating nanoparticles in lung metastases. Nat. Biomed. Eng. 5, 441–454 (2021).
He, Y. et al. Intravenous senescent erythrocyte vaccination modulates adaptive immunity and splenic complement production. ACS Nano 18, 470–482 (2024).
















Leave a Reply